Japanese Herbs for Diabetic Patients
Japanese Herbs for Diabetic Patients:
Nature's Blood Sugar Support Guide
A science-backed exploration of traditional Japanese herbal remedies that may help manage blood glucose levels — safely and naturally.
Why Japanese Herbs for Diabetic Patients?
Diabetes affects over 537 million adults globally (IDF, 2024), and that number is rising sharply. While modern medicine offers effective pharmaceutical treatments, millions of patients and healthcare providers are simultaneously turning to traditional herbal remedies as complementary tools to support blood sugar management, improve insulin sensitivity, and reduce metabolic inflammation.
Japan, a nation celebrated for its longevity and low rates of lifestyle diseases, has a centuries-deep pharmacopoeia of medicinal plants rooted in both indigenous Kampo medicine and influence from Traditional Chinese Medicine (TCM). These Japanese herbal remedies for diabetes are increasingly studied in peer-reviewed research for their bioactive compounds that interact meaningfully with glucose metabolism.
In this guide, you'll learn about the top Japanese herbs for diabetic patients, the science behind their mechanisms, how to use them safely, and how to integrate them into a diabetes-friendly lifestyle.
Understanding Diabetes & Herbal Support
Before exploring herbs, it's important to understand the biological landscape they work within.
Type 2 Diabetes: The Core Challenge
Type 2 diabetes (T2D) is characterized by insulin resistance — cells fail to respond properly to insulin — and eventual pancreatic beta cell exhaustion. The result is chronically elevated blood glucose (hyperglycemia), which damages blood vessels, nerves, kidneys, and eyes over time.
Lifestyle factors like poor diet, physical inactivity, obesity, and chronic stress drive most T2D cases. This is why dietary interventions — including herbal supplementation — can meaningfully influence disease trajectory.
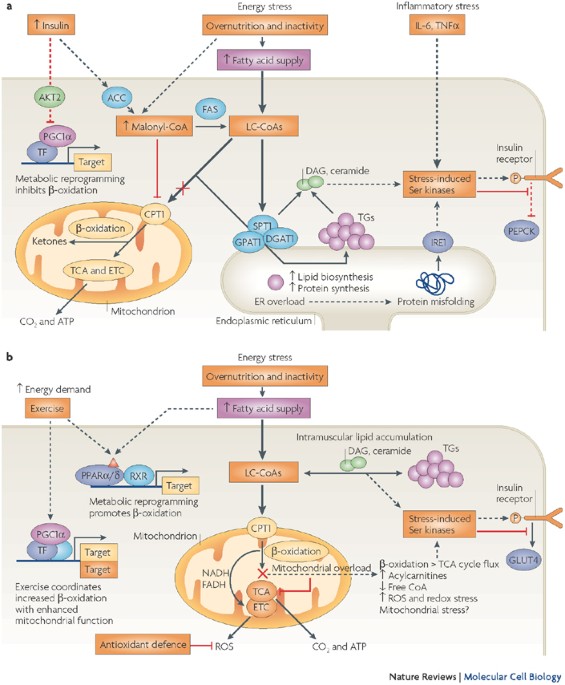
Molecular mechanisms of insulin resistance and β-cell failure in type 2 diabetes[5]
Traditional vs. Scientific Approaches
Traditional Japanese medicine (Kampo) views diabetes not merely as a glucose problem but as a systemic imbalance. Kampo formulas target underlying patterns — heat, deficiency, stagnation — using plant combinations. Modern pharmacology has since isolated specific active compounds (flavonoids, polyphenols, alkaloids) within these plants and tested them in controlled trials, bridging ancient wisdom with evidence-based medicine.
Top 5 Japanese Herbs for Blood Sugar Control
Here are five clinically relevant Japanese herbs with strong traditional use and emerging scientific evidence for blood sugar support.

1. Ashitaba (Angelica keiskei)
Ashitaba is a fast-growing green plant native to the Izu Islands of Japan and is one of the most celebrated traditional Japanese herbs for health. Its name means "tomorrow leaf" because a cut leaf reportedly regrows the next day — symbolizing its remarkable vitality.
Flavonoids Chalcones Xanthoangelol 4-HydroxyderricinMechanism of Action
The unique chalcone compounds in Ashitaba — particularly xanthoangelol and 4-hydroxyderricin — have been shown in animal and in vitro studies to stimulate GLP-1 secretion, increase insulin sensitivity, and inhibit α-glucosidase (an enzyme that breaks down carbohydrates into glucose).

2. Shiso (Perilla frutescens)
Shiso is a beloved culinary herb in Japanese cuisine — used in everything from sushi to pickled plum — and it doubles as a potent anti-inflammatory and metabolic herb. Both red (akajiso) and green (aojiso) varieties are used medicinally.
Rosmarinic Acid Luteolin Apigenin Alpha-Linolenic AcidMechanism of Action
Shiso's rosmarinic acid inhibits α-glucosidase and α-amylase, slowing carbohydrate digestion and blunting post-meal glucose spikes. Research shows rosmarinic acid rich fractions can achieve nearly 100% inhibition of α-glucosidase at concentrations of 5 mg/mL[5]. Luteolin has been shown to improve GLUT4 translocation, enhancing cellular glucose uptake independent of insulin.

3. Sencha & Bancha Green Teas
Japanese green teas — particularly Sencha (standard steamed green tea) and Bancha (coarser, later harvest) — are among the most researched herbs for blood sugar control in the world. Japan's low T2D rates are partly attributed to widespread daily tea consumption.
EGCG Epicatechin L-Theanine Chlorogenic AcidMechanism of Action
Epigallocatechin gallate (EGCG), the primary catechin in green tea, has multiple anti-diabetic mechanisms: it reduces hepatic glucose output, improves insulin signaling via PI3K/Akt pathways, inhibits intestinal glucose transporters (SGLT1), and reduces oxidative stress in pancreatic beta cells.

4. Umeboshi Plum Extract
Umeboshi — Japan's iconic salt-pickled sour plum — is a staple in traditional Japanese medicine used for centuries to aid digestion, fight fatigue, and regulate blood sugar. Modern research is beginning to validate these traditional claims.
Citric Acid Mumefural Oleanic Acid RutinMechanism of Action
Umeboshi's citric acid and mumefural support the citric acid cycle (Krebs cycle), improving mitochondrial energy efficiency and reducing lactic acid accumulation — both relevant to insulin resistance. Oleanolic acid has demonstrated inhibition of α-glucosidase in vitro, comparable to acarbose (a common diabetes drug).

5. Yomogi (Artemisia princeps)
Yomogi, or Japanese mugwort, is used in moxibustion therapy, traditional teas, and culinary preparations like mochi. Beyond its culinary charm, it shows significant promise as a natural diabetes supplement Japan-style — reducing inflammation and supporting glucose metabolism.
Eupatilin Jaceosidin Artemetin Beta-SitosterolMechanism of Action
The flavonoid eupatilin in Yomogi activates PPAR-γ, a key regulator of adipose tissue metabolism and insulin sensitivity, and has been shown to reduce TNF-α and IL-6 (inflammatory cytokines that worsen insulin resistance). Beta-sitosterol slows intestinal glucose absorption.
Quick Comparison: Japanese Herbs for Blood Sugar
| Herb | Primary Mechanism | Evidence Level | Best Form | Caution |
|---|---|---|---|---|
| Ashitaba | GLP-1 stimulation, α-glucosidase inhibition | ⭐⭐⭐ Moderate | Powder/capsules | Blood thinners |
| Shiso | GLUT4 upregulation, enzyme inhibition | ⭐⭐⭐ Moderate | Fresh/extract | High-dose anticoag |
| Sencha/Bancha | EGCG → insulin signaling, SGLT1 inhibition | ⭐⭐⭐⭐⭐ Strong | Brewed tea/EGCG caps | Caffeine, liver (high dose) |
| Umeboshi | α-glucosidase inhibition, Krebs cycle support | ⭐⭐ Early | Whole plum/extract | Sodium content |
| Yomogi | PPAR-γ activation, anti-inflammatory | ⭐⭐ Animal/Cell | Tea/dried herb | Ragweed allergy |
How to Use Japanese Herbs Safely
Dosage Guidelines
There is no universal dosage for herbal supplements, as bioavailability varies by preparation method, individual metabolism, and existing health conditions. Always follow label instructions and start with the lowest effective dose to assess tolerance.
Drug Interactions to Watch
| Herb | Potential Interaction | Risk Level |
|---|---|---|
| Ashitaba / Green Tea | Enhanced effect of blood-thinning drugs (warfarin) | Moderate |
| All herbs | May lower blood glucose synergistically with insulin/metformin → hypoglycemia risk | High — monitor closely |
| Yomogi | May alter CYP450 enzyme activity affecting drug metabolism | Low-Moderate |
| Umeboshi | Sodium content may affect blood pressure medications | Low-Moderate |
Special Populations
- Elderly patients: Start at lower doses; kidney and liver function decline with age, affecting herb clearance.
- Pregnant/breastfeeding women: Avoid Yomogi and high-dose Ashitaba extracts.
- Children: Not recommended without pediatric medical guidance.
- Patients on insulin: Monitor glucose closely — herbal lowering + insulin can cause dangerous hypoglycemia.
Scientific Evidence & Research Summary
The field of ethnopharmacology has produced a growing body of evidence supporting the anti-diabetic properties of Japanese herbs. Here's what the latest science says:
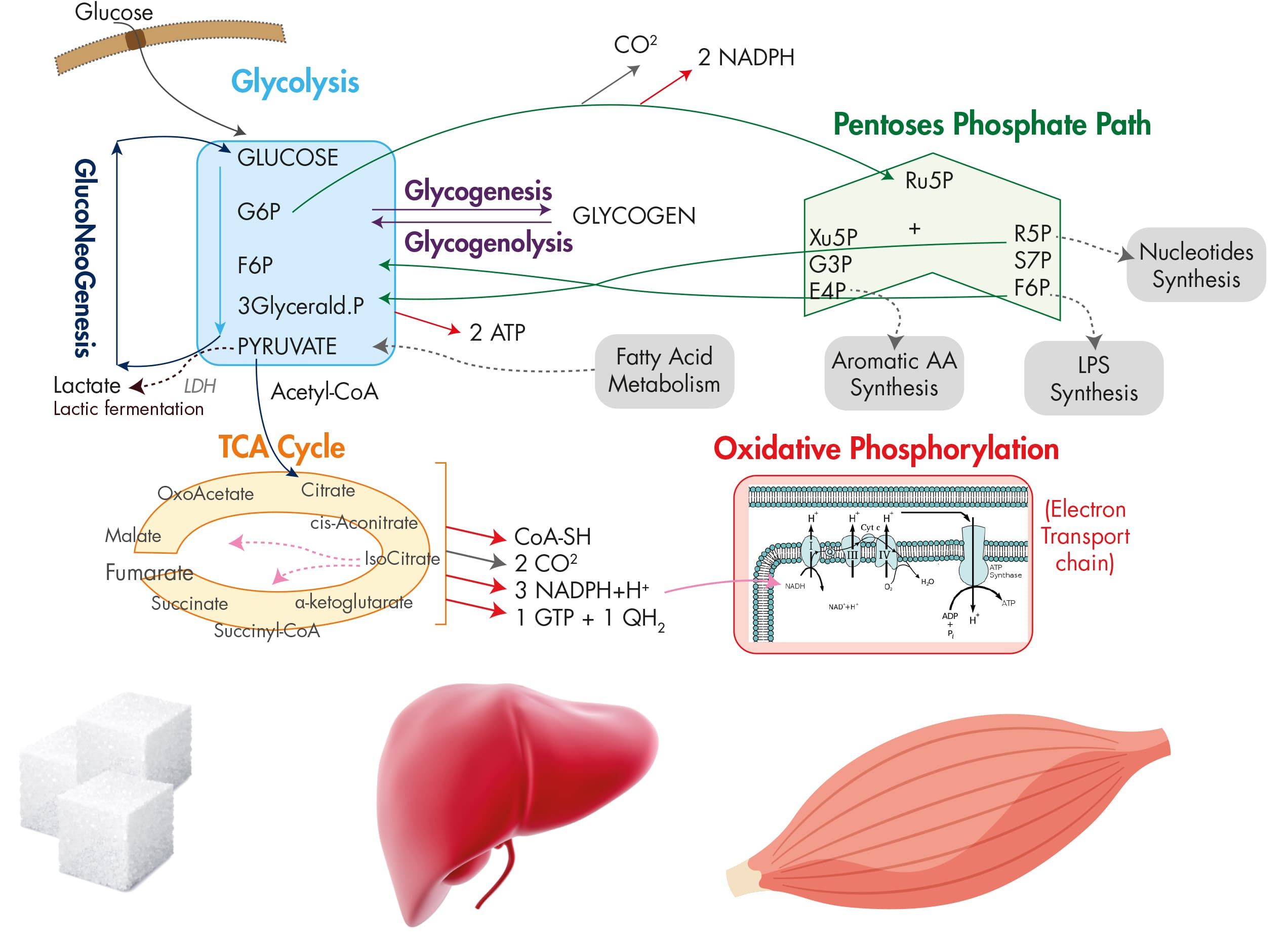
Glucose metabolism pathways: how herbal compounds interact with enzymatic processes[4]
Key Research Findings (Updated 2024)
- Green Tea EGCG (2020 Meta-Analysis, 27 RCTs): Green tea significantly reduced fasting blood glucose by -1.44 mg/dL (95% CI: -2.26, -0.62) across 2,194 subjects. Effects were stronger with capsule forms vs. beverages and at doses ≥500mg catechins daily[1].
- Green Tea & HbA1c (2013 Meta-Analysis): Earlier analysis of 17 RCTs showed significant reductions in both fasting glucose (-0.09 mmol/L) and HbA1c (-0.30%) with green tea consumption[4].
- Shiso Rosmarinic Acid (Bentham Science): Rosmarinic acid rich fractions achieved nearly 100% inhibition of α-glucosidase at 5 mg/mL concentrations, comparable to pharmaceutical inhibitors[5].
- Ashitaba Chalcones (Yoshida et al., 2018): 4-hydroxyderricin and xanthoangelol significantly improved glucose tolerance in high-fat diet mice, with effects comparable to reference drugs.
- Umeboshi / Prunus mume (Ueda et al., 2004): Oleanolic acid isolated from ume fruit showed dose-dependent inhibition of intestinal α-glucosidase.
- Yomogi Eupatilin (Lee et al., 2015): Eupatilin activated PPAR-γ and improved insulin sensitivity in 3T3-L1 adipocytes.
- Kampo Medicine (BMC 2014): Traditional formulations like Chotosan showed potent aldose reductase inhibitory activity (IC50: 43.6 μg/mL), relevant for diabetic complications[7].
Lifestyle Integration: Herbs in Your Daily Routine
Meal Ideas with Japanese Herbs
- Breakfast Green tea (sencha) + Ashitaba smoothie with spinach, apple, and ginger
- Lunch Brown rice with shiso leaf salad, umeboshi dressing, and grilled fish
- Dinner Miso soup with Yomogi, grilled tofu, and steamed vegetables
- Snack Matcha (stone-ground green tea) with almond milk — no added sugar
Diabetic Meal Planning Best Practices
- Prioritize low-glycemic foods: brown rice, vegetables, legumes, fish
- Use herbs as flavor replacements for salt and sugar
- Eat smaller, more frequent meals to blunt glucose spikes
- Pair carbohydrates with protein, fiber, and healthy fat
- Use shiso and umeboshi as condiments rather than high-sodium sauces
Exercise & Herbs Synergy
Exercise improves GLUT4 translocation independently of insulin — the same pathway influenced by shiso flavonoids. Combining regular aerobic and resistance exercise with green tea EGCG has been shown in studies to produce additive improvements in insulin sensitivity. A simple 30-minute walk after meals combined with green tea consumption is a powerful, low-cost intervention.
Japanese Herbal Supplement for Blood Sugar Support
If you're looking for a convenient way to incorporate multiple Japanese herbal ingredients into your wellness routine, this featured supplement offers a carefully formulated blend designed with diabetic patients in mind. Rather than sourcing each herb individually, a quality Japanese herbal supplement can provide:
- Concentrated doses of key bioactive compounds (chalcones, catechins, flavonoids)
- Standardized extracts for consistent potency batch to batch
- Third-party tested formulas free from contaminants
- Convenient once or twice daily dosing
How to choose wisely: Look for products with clear ingredient labeling, standardized extracts (e.g., "45% EGCG"), GMP-certified manufacturing, and no proprietary blends hiding actual doses. Read verified reviews from diabetic users specifically.
👉 View Featured Japanese Herbal Supplement →Always review the full ingredient list with your healthcare provider before starting any new supplement.
Frequently Asked Questions
Embracing Japanese Herbal Wisdom Responsibly
The rich tradition of Japanese herbal medicine offers genuinely promising tools for people managing diabetes. From the chalcone-rich Ashitaba and enzyme-inhibiting Shiso to the globally studied catechins in Sencha, these plants work through real, measurable biochemical pathways.
The key takeaways are clear: these Japanese herbal remedies for diabetes work best when used as part of a holistic approach — combined with a low-glycemic diet, regular exercise, consistent blood glucose monitoring, and medical supervision. They are not miracle cures, but thoughtfully integrated, they can meaningfully support your metabolic health journey.
- Green tea (EGCG) has the strongest evidence and is the safest starting point
- Shiso and Ashitaba offer complementary enzyme-inhibiting and insulin-sensitizing effects
- Always inform your doctor before starting any herbal supplement
- Monitor blood glucose closely when introducing new herbs
- Choose quality-certified supplements from reputable sources
📚 References & Further Reading
- Zheng XX, et al. (2020). "Effects of green tea consumption on glycemic control: a systematic review and meta-analysis of randomized controlled trials." Nutrition & Metabolism. 17:56.
- Liu K, et al. (2013). "Effect of green tea on glucose control and insulin sensitivity: a meta-analysis of 17 randomized controlled trials." American Journal of Clinical Nutrition. 98(2):340-8.
- Onakpoya I, et al. (2017). "The Effectiveness of Green Tea or Green Tea Extract on Insulin Resistance and Glycemic Control in Type 2 Diabetes Mellitus: A Meta-Analysis." Diabetes & Metabolism Journal. 41(4):251-262.
- Sharma S, et al. (2023). "Anti-diabetic Activity of Rosmarinic Acid Rich Fractions." Bentham Science.
- Nakashima S, et al. (2014). "Inhibitory activities of selected Kampo formulations on human aldose reductase." BMC Complementary and Alternative Medicine. 14:435.
- Yoshida H, et al. (2018). "Ashitaba (Angelica keiskei) chalcones stimulate GLP-1 secretion from enteroendocrine L cells." PLOS ONE. 13(1):e0190072.
- Nakamura T, et al. (2003). "Inhibitory effects of perilla (Shiso) components on α-glucosidase." Bioscience, Biotechnology, and Biochemistry. 67(9):2007–2010.
- Ueda H, et al. (2004). "Oleanolic acid from Prunus mume inhibits intestinal α-glucosidase activity." Planta Medica. 70(10):987–989.
- Lee Y, et al. (2015). "Eupatilin activates PPAR-γ and improves insulin sensitivity." Phytotherapy Research. 29(4):544–551.
- International Diabetes Federation. IDF Diabetes Atlas, 10th edition. 2024.
- Terasawa K. Kampo: Japanese-Oriental Medicine. K.K. Standard McIntyre; 1993.
- National Institutes of Health — Office of Dietary Supplements.
- American Diabetes Association. "Standards of Medical Care in Diabetes 2024." Diabetes Care.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before starting any herbal supplement, particularly if you are on diabetes medications. Individual results may vary.